Lesson 13
1 Learning Objectives
By the end of this lesson students will be able to:
- Manipulate block diagrams
- Define and calculate open-loop gain, loop gain, open-loop transfer function, and closed-loop transfer function
- Draw control system diagrams from a description of a system
2 Block Diagram Manipulation
Blocks in series can be multiplied together.
Blocks in parallel can be added within a single block.
Build general-purpose equations by combining multiplication and addition, like this:
Lastly, what does this mean about single blocks? Can they be split up into many?
3 Open and Closed-Loop Systems
3.1 Open Loop
Consider a fan heater that is used to heat a room. The block diagram might look like this:
We can write the transfer function of this system as
Since the input is multiplied by , we call this the open-loop gain, or OLG.
- Remember, the drawback to an open-loop system is that it does not know when a desired output has been reached.
3.2 Closed Loop
Now, suppose we throw away our fan heater and buy a new one that will shut off once the room hits a certain temperature. The block diagram might look like:
3.3 Student Exercise 1
Derive the equation for the transfer function of this system.
The product is called the loop gain (LG) or open-loop transfer function because it is the product of all the gains in the feedback loop. This equation is different from OLG!
In control system terminology, is referred to as the closed-loop transfer function. The closed-loop transfer function is the entire closed-loop system compressed into a single block.
4 Steady-State Operating Point of Physiological Systems
Physiological control systems do not have reference inputs or error detectors. For example, there are no knobs on your body to adjust blood glucose or body temperature. So how is the body able to regulate these things?
The idea of a steady-state operating point, or equilibrium, provides a method for determining the reference point of physiological systems.
4.1 Example 1
Draw a block diagram for the control of carbon dioxide levels in the blood. The medullary respiratory center senses levels in the blood (via H ions generated from dissociating carbonic acid) and adjusts the rate of neural impulses to the chest and lung muscles to increase or decrease alveolar ventilation rate . This in turn affects the levels of the blood.
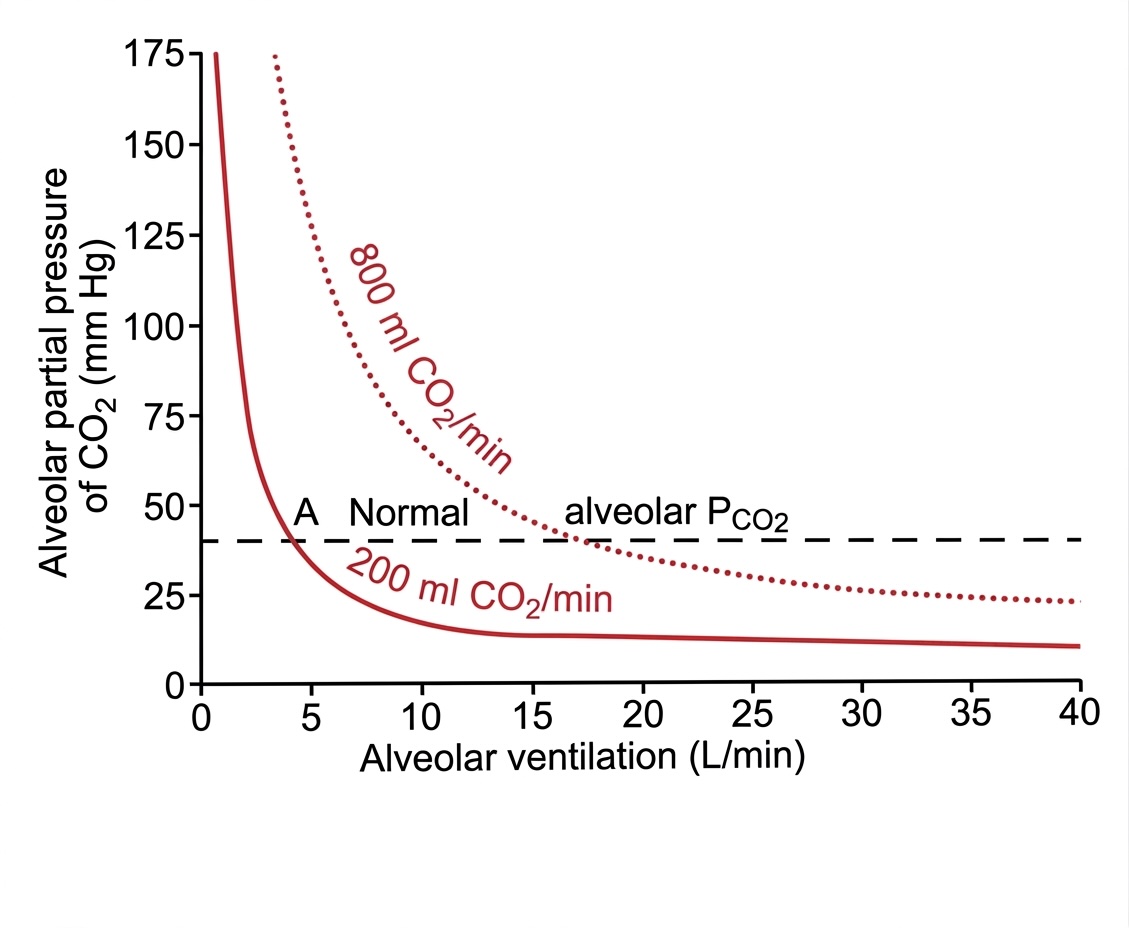
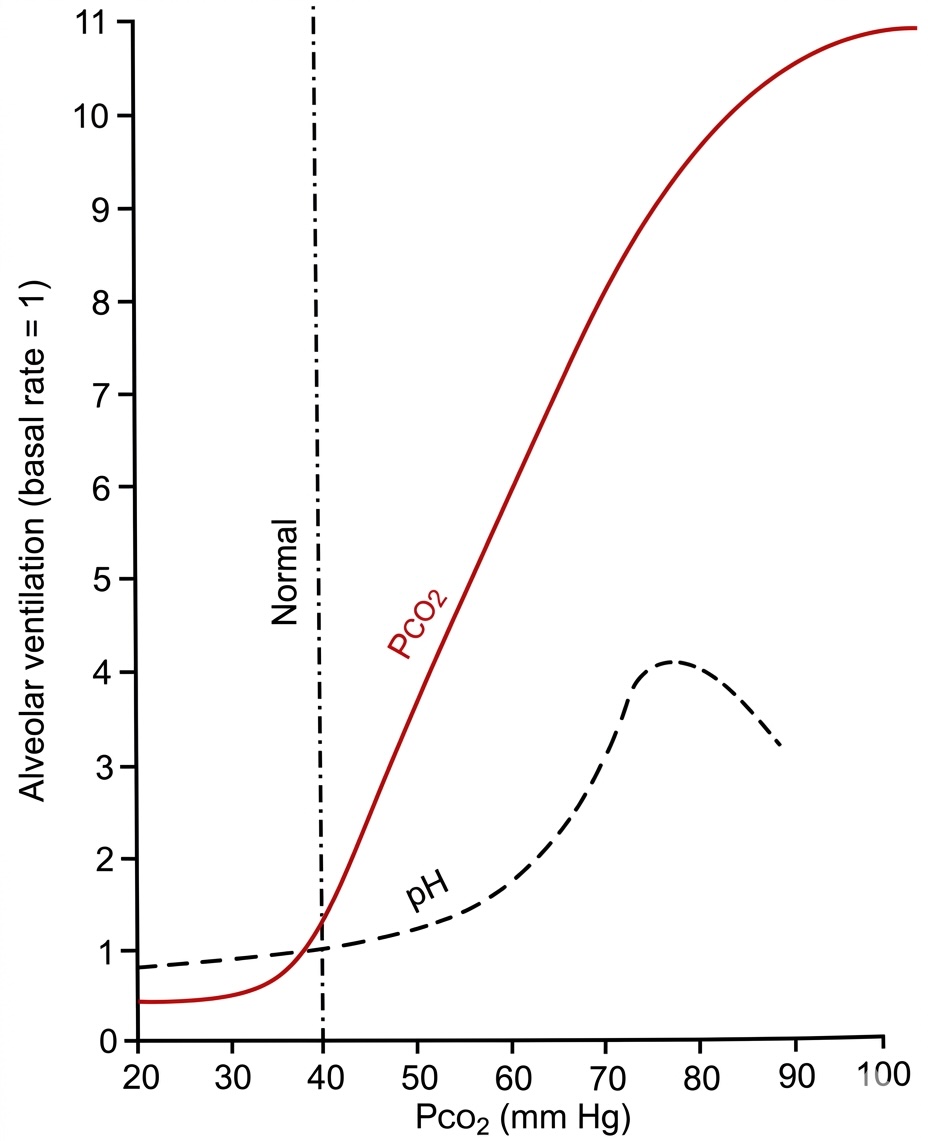
Where is the reference point though? In other words, where will the system settle down to under normal operating conditions?
Why does the system settle at one point?
4.2 Student Exercise 2
Regulation of sodium. Sodium ions need to be regulated because small variations in their concentration can cause drastic changes in bodily function. Sodium seems to be actively reabsorbed by all segments of the renal tubules. It may be almost completely reabsorbed or, on the other hand, it may fail to be reabsorbed and large portions pass into the urine. The variability of sodium reabsorption is controlled by the aldosterone concentration of the extracellular fluid. According to one theory, if sodium concentration falls it causes the diencephalon (which contains the hypothalamus, thalamus, etc.) to increase the secretion rate of glomerulotropin. Increased glomerulotropin levels cause an increase in the secretion rate of aldosterone from the adrenal cortex, thereby raising the extracellular fluid concentration of this hormone. This, then, acts on the kidney tubules to increase the reabsorption rate of sodium ions.
4.3 Student Exercise 3
Regulation of calcium. A low level of calcium ion concentration in the extracellular fluid can lead to tetanic contraction of muscles and death due to respiratory paralysis. As calcium ion concentration in the extracellular fluid decreases, parathyroid hormone (PTH) is released which acts on the bone salts and releases stored calcium. Increased PTH also results in increased calcium ion reabsorption by the renal tubules which increases extracellular concentration of calcium.
4.4 Student Exercise 4
Regulation of extracellular fluid osmolarity. The regulation of extracellular fluid (ECF) osmolarity is vested in the so-called osmoreceptor-antidiuretic hormone system. A high ECF osmolarity causes the hypothalamus to send increased nerve impulses to the neurohypophysis (posterior pituitary gland), which causes secretion of antidiuretic hormone (ADH). ADH promotes increased water reabsorption from the distal tubules and collecting ducts. This, in turn, results in a reduced ECF osmolarity.
Special ganglion cells, known as osmoreceptors, are located in the anterior hypothalamus and respond to changes in ECF osmolarity. These cells supposedly contain large fluid chambers which are filled with ECF and each of which continually emits nerve impulses. When the ECF osmolarity becomes very low, osmosis of the water into the fluid chambers of the osmoreceptors causes them to swell, which decreases their rate of impulse discharge. The impulses are transmitted through the pituitary stalk into the neurohypophysis where they cause the release of ADH.
4.5 Student Exercise 5
Regulation of arterial pressure. There are three basic mechanisms by which the arterial pressure is normally regulated. (1) If all pressures throughout the circulatory system become very high, fluid begins to leak from the capillaries into the interstitial spaces. This decreases the blood volume and lowers the arterial pressure until the capillary pressure returns almost to normal. (2) The autonomic nervous system regulates the activity of the heart and the degree of constriction of the blood vessels throughout the body, thus affecting arterial pressure. High heart rate and an increase in total peripheral resistance increase arterial pressure. (3) The kidneys help regulate arterial pressure. When the arterial pressure becomes too low, the kidneys, either by altering the body fluids or by causing constriction of arterioles throughout the body, elevate the arterial pressure back to normal. Arterioles are restricted by the release of renin. Conversely, if the pressure rises too high, the kidneys promote appropriate circulatory changes to decrease the pressure to normal.